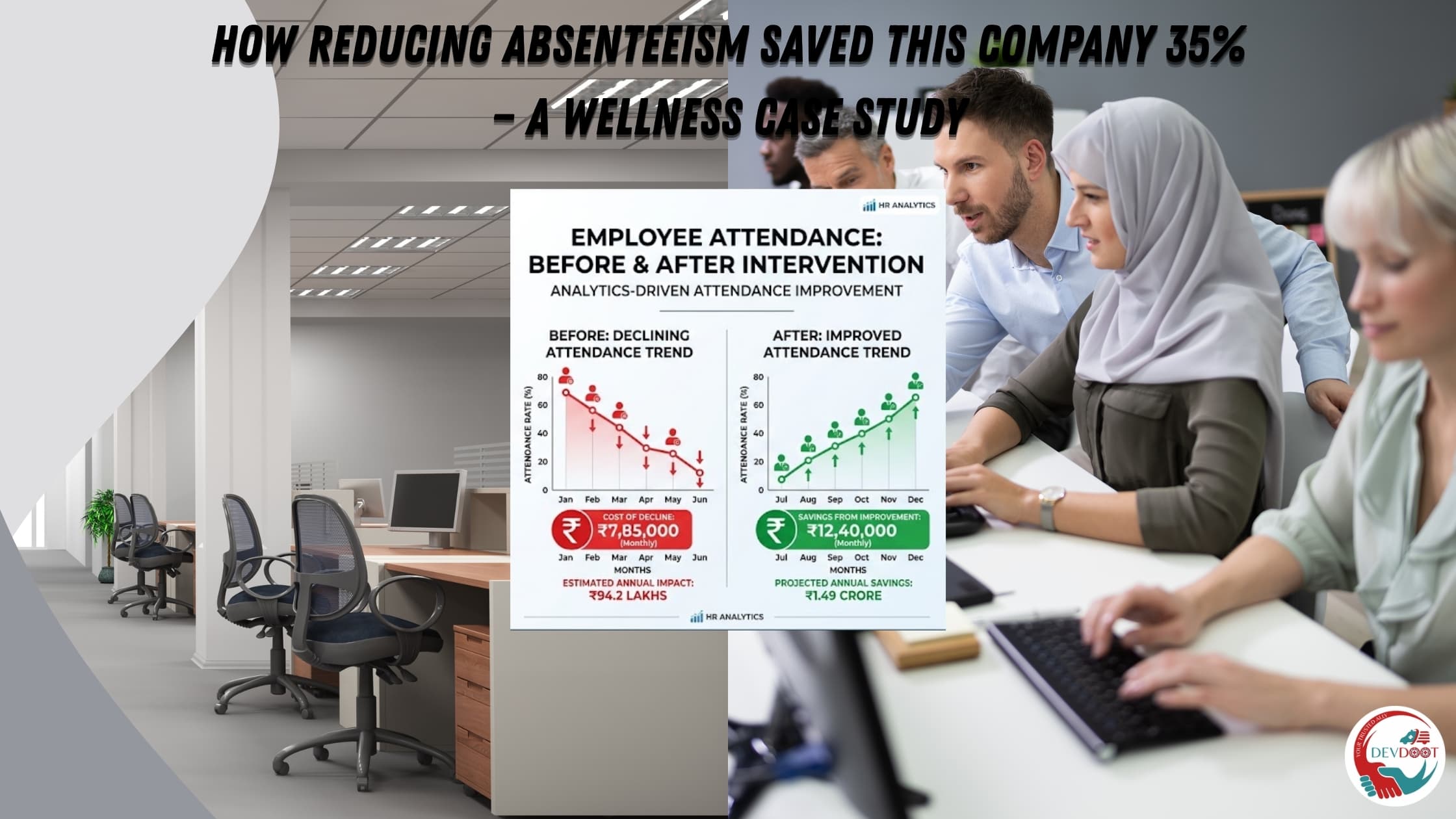
The numbers from this case study are real, though we have anonymized the company at their request. It is a mid-size BFSI organization headquartered in Pune, 840 employees, with a chronic absenteeism problem that had worsened year-over-year for three years before they decided to address the root cause rather than the symptom.
The Problem
In FY 2022–23, the organization recorded 7.8 average unplanned absence days per employee — nearly double the 4.2-day BFSI sector benchmark. Finance calculated the direct cost at Rs 2.1 crore annually (replacement labor, project delays, manager time managing coverage). This figure excluded the harder-to-quantify costs: client relationship disruption, team morale decline, and the compounding effect of high performers carrying absent colleagues' workloads.
HR had tried standard interventions: attendance improvement plans, manager coaching, and flexible work policies. Absenteeism came down slightly in Q1 after each intervention, then returned to baseline. The interventions treated absence as a behavioral problem. It was actually a health problem.
The Diagnosis
A confidential health risk assessment in Q1 FY 2023–24 found the following: 58% of employees reported chronic physical health issues contributing to absence (primarily musculoskeletal pain and digestive issues); 44% reported mental health factors including anxiety, depression, and burnout driving absence behavior; 37% reported financial stress as a significant factor in overall wellbeing degradation. Critically, 71% said they had not accessed any health support through the company because they did not know it existed or did not trust the process.
The Solution
The organization launched a three-pillar wellness program in Q2 FY 2023–24. Pillar one: physical health — weekly on-site physiotherapy sessions (addressing the back and neck pain majority), nutrition guidance, and preventive health screening. Pillar two: mental health — a digital-first counseling and stress management platform with anonymous access, covering the 44% of employees with mental health-related absence drivers. Pillar three: financial wellness — a fortnightly financial planning workshop series and access to an emergency financial assistance fund for genuine crisis cases.
Crucially, they ran a parallel manager training program — eight hours over two sessions — covering how to identify early signs of employee distress, how to have supportive conversations about wellbeing without overstepping, and how to signpost employees to available support resources.
The Results
By Q4 FY 2023–24 (nine months after launch), unplanned absence days per employee had dropped from 7.8 to 5.1 — a 35% reduction. The direct cost saving was Rs 72 lakh annually. Secondary results included eNPS improvement from +12 to +29, voluntary turnover reduction from 18% to 13%, and a 19% reduction in healthcare insurance claims in the same period.
The program cost Rs 18 lakh in year one (platform, on-site services, training). Against Rs 72 lakh in direct absenteeism savings, plus secondary savings from reduced turnover and lower insurance costs, the year-one ROI was approximately 4:1.
Lessons Learned
Three lessons from this case. First, treat absenteeism as a health signal, not a behavioral problem. Absence improvement plans address behavior; wellness programs address causes. Second, multi-pillar programs outperform single-intervention programs. Physical health, mental health, and financial wellness all contributed meaningfully. No single pillar would have achieved 35% reduction alone. Third, manager enablement is non-negotiable. The most impactful single driver in this case was managers who spotted early distress signals and directed employees to support before absence occurred.
Conclusion
The numbers from this case are not exceptional — they reflect what structured wellness programs routinely achieve when they address root causes and measure the right outcomes. If your organization has chronic absenteeism, the question is not whether wellness can help. It is whether you are ready to measure it properly.